ADHD and Emotional Dysregulation – What Does the Research Say?
ADHD and emotional regulation are closely connected for many children in school settings. While inattention and hyperactivity are the most recognized signs of ADHD, difficulties managing emotions are also a common and significant part of how this condition shows up in daily life. These emotional challenges can affect how children perform in class, interact with peers, and respond to adults across the school day.
A 2026 study published in Psychological Medicine examined brain structure and function in young children with ADHD, with a specific focus on those who also experienced impairing emotional outbursts. The findings suggest that emotional dysregulation in ADHD may involve distinct brain patterns that are worth understanding for anyone who works with these children.

WHAT THE RESEARCH EXAMINED
Researchers from the Child Mind Institute and Fordham University studied brain structure and connectivity in young children to better understand what makes ADHD with emotional outbursts different from ADHD without them.
Key study details:
- 123 children ages 5 to 9.9 years participated
- Three groups were compared: children with ADHD and impairing emotional outbursts (ADHD + IEO, n = 47), children with ADHD only (n = 39), and neurotypical controls (n = 37)
- Impairing emotional outbursts were defined as severe verbal or physical rages occurring at least three times per week, lasting at least 15 minutes on average, for at least six months
- Brain scans measured cortical thickness and resting-state functional connectivity
- Parent-report questionnaires assessed behavior, temperament, and emotion regulation
- Data-driven statistical methods were used to identify patterns rather than relying on preselected brain regions
KEY FINDINGS FROM THE RESEARCH
The study found that children with ADHD and impairing emotional outbursts showed distinct behavioral and brain patterns compared to children with ADHD alone and neurotypical peers.
Specific findings include:
- Four behavioral patterns were identified through analysis of parent-report questionnaire data: externalizing behavior, emotion dysregulation, internalizing behavior, and surgency/impulsivity
- The externalizing behavior pattern was significantly more pronounced in the ADHD + IEO group than in both the ADHD and neurotypical groups
- Children with ADHD + IEO showed greater cortical thickness in the left dorsolateral prefrontal cortex compared to neurotypical controls; this brain region is associated with executive control and emotion regulation
- Thicker cortex in this region was significantly associated with higher externalizing behavior scores
- Children with ADHD + IEO showed reduced connectivity between the DLPFC and regions of the default mode network compared to neurotypical controls.
- The ADHD + IEO group also showed reduced connectivity in visual, dorsal attention, and salience networks compared to the ADHD-only group, suggesting these patterns may be more specific to emotional dysregulation than to ADHD broadly
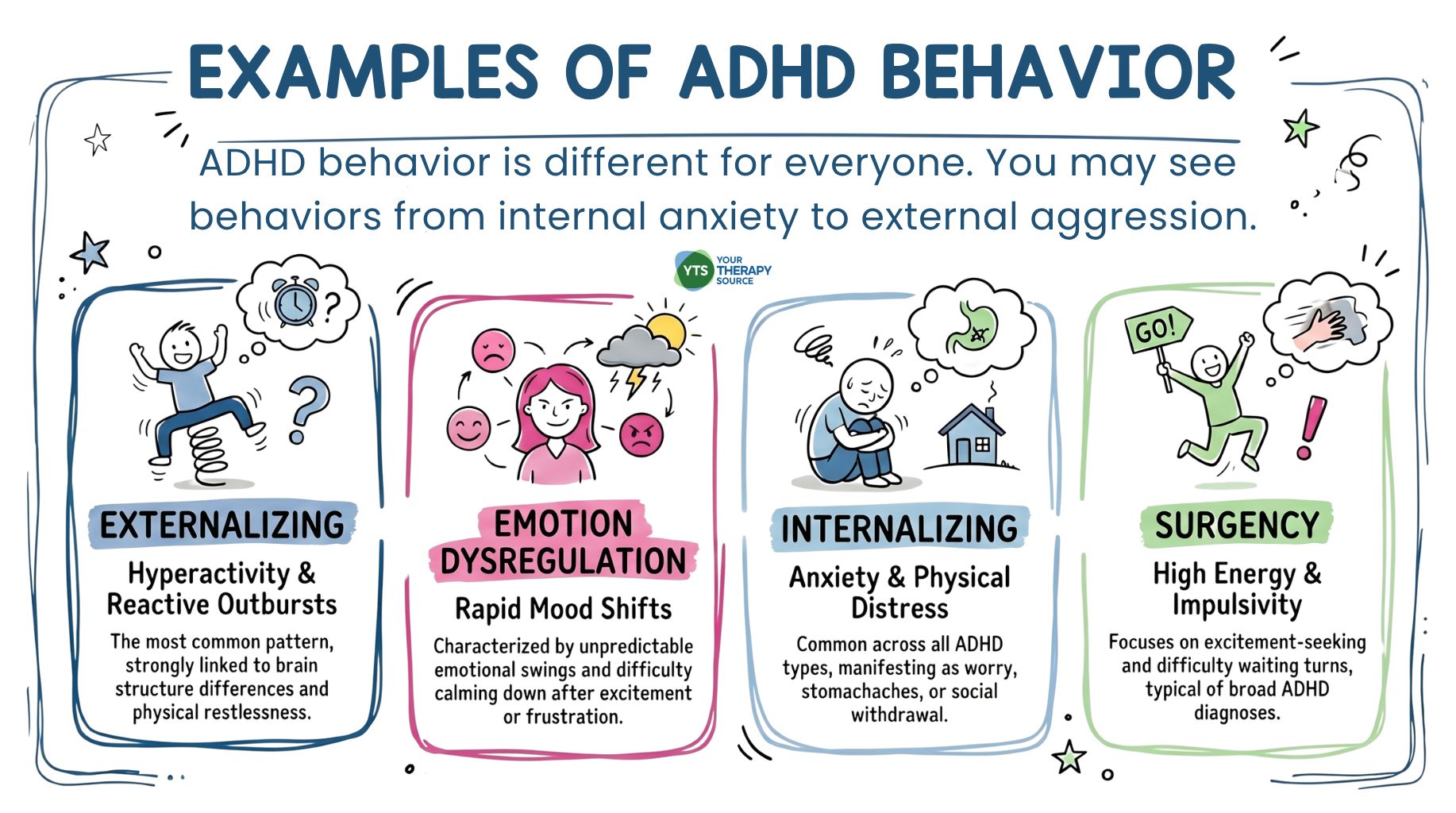
THE FOUR BEHAVIORAL PATTERNS IDENTIFIED
One of the study’s key contributions is the identification of four distinct behavioral patterns through parent-report data. Understanding these patterns can help school professionals recognize the range of ways dysregulation shows up in children with ADHD.
Pattern 1: Externalizing Behavior
- Captured hyperactivity, anger, aggression, and related externalizing problems
- The dominant pattern in the study and the one most strongly linked to brain structure and connectivity differences
- Children with ADHD + IEO scored significantly higher on this pattern than both children with ADHD alone and neurotypical peers, with a very strong effect size separating those groups
- In school settings, this may look like difficulty staying seated, reactive outbursts toward peers or adults, and trouble recovering after conflict
Pattern 2: Emotion Dysregulation
- Focused on items related to impairing emotional outbursts and both positive and negative emotion dysregulation
- Included measures of tantrum behavior such as high anger, low anger, and distress, as well as emotion lability
- Children with ADHD + IEO scored higher on this pattern than children with ADHD alone; no other group differences were significant
- This suggests the pattern captures something specific to children who experience severe outbursts rather than ADHD broadly
- In school settings, this may look like rapid shifts between emotional states, difficulty calming after excitement or frustration, or reactions that feel unpredictable to staff and peers
Pattern 3: Internalizing Behavior
- Captured anxiety, somatization, and other internalizing symptoms
- Both the ADHD + IEO and ADHD-only groups scored significantly higher on this pattern than neurotypical peers, but there was no significant difference between the two ADHD groups
- This suggests internalizing difficulties are broadly associated with ADHD regardless of whether a child also experiences severe emotional outbursts
- In school settings, this may present as worry, stomachaches before tests or transitions, social withdrawal, or difficulty expressing distress verbally
Pattern 4: Surgency and Impulsivity
- Had the lowest factor loadings overall and included items related to positive affect, impulsivity, and surgency, which refers to high energy, excitement-seeking, and rapid approach behavior
- Children with ADHD alone scored higher on this pattern than neurotypical peers; no other group differences were significant
- This suggests the pattern is more characteristic of ADHD broadly than of the subset of children who also experience impairing emotional outbursts
- In school settings, this can appear as difficulty waiting turns, moving quickly from one activity to another, or becoming overly excited in stimulating environments
WHY THESE FINDINGS MATTER FOR SCHOOL-BASED PRACTICE
These findings suggest that emotional dysregulation in ADHD is not simply an extension of behavioral difficulties. It may involve different brain-level patterns that go beyond what is typically captured in an ADHD diagnosis alone.
Key points for school-based practice:
- Children who show both ADHD symptoms and frequent, severe emotional outbursts may have more complex support needs than children with ADHD without those outbursts
- The brain regions involved are linked to executive function, attention, and the processing of emotionally meaningful information, all of which are relevant to classroom learning and participation
- Emotional dysregulation in young children with ADHD may not be fully captured by behavioral observation alone, pointing to the value of multimodal assessment and close collaboration with families
Understanding how sensory needs in ADHD and emotional regulation intersect can help school teams build a more complete picture of a child’s experience.
IMPLICATIONS FOR SCHOOL STAFF
This research suggests that children with ADHD who also show significant emotional outbursts may experience challenges that are distinct from those of children with ADHD alone. School staff are often the first to observe these patterns across the day.
Staff may notice students who:
- React with intense emotional responses that seem disproportionate to the situation
- Struggle to recover after an emotional outburst and return to learning tasks
- Have difficulty shifting attention or self-regulating after a stressful interaction
- Show different patterns of dysregulation in structured versus unstructured settings
Understanding that these behaviors may reflect underlying differences in brain connectivity can help staff respond with greater consistency. A multi-modal support approach, one that addresses sensory processing, self-regulation, executive function, and emotional needs together, tends to be more effective than targeting behavior in isolation. Exploring connections between sensory processing and learning can be one useful part of that broader picture.



10 PRACTICAL STRATEGIES FOR ADHD AND EMOTIONAL DYSREGULATION
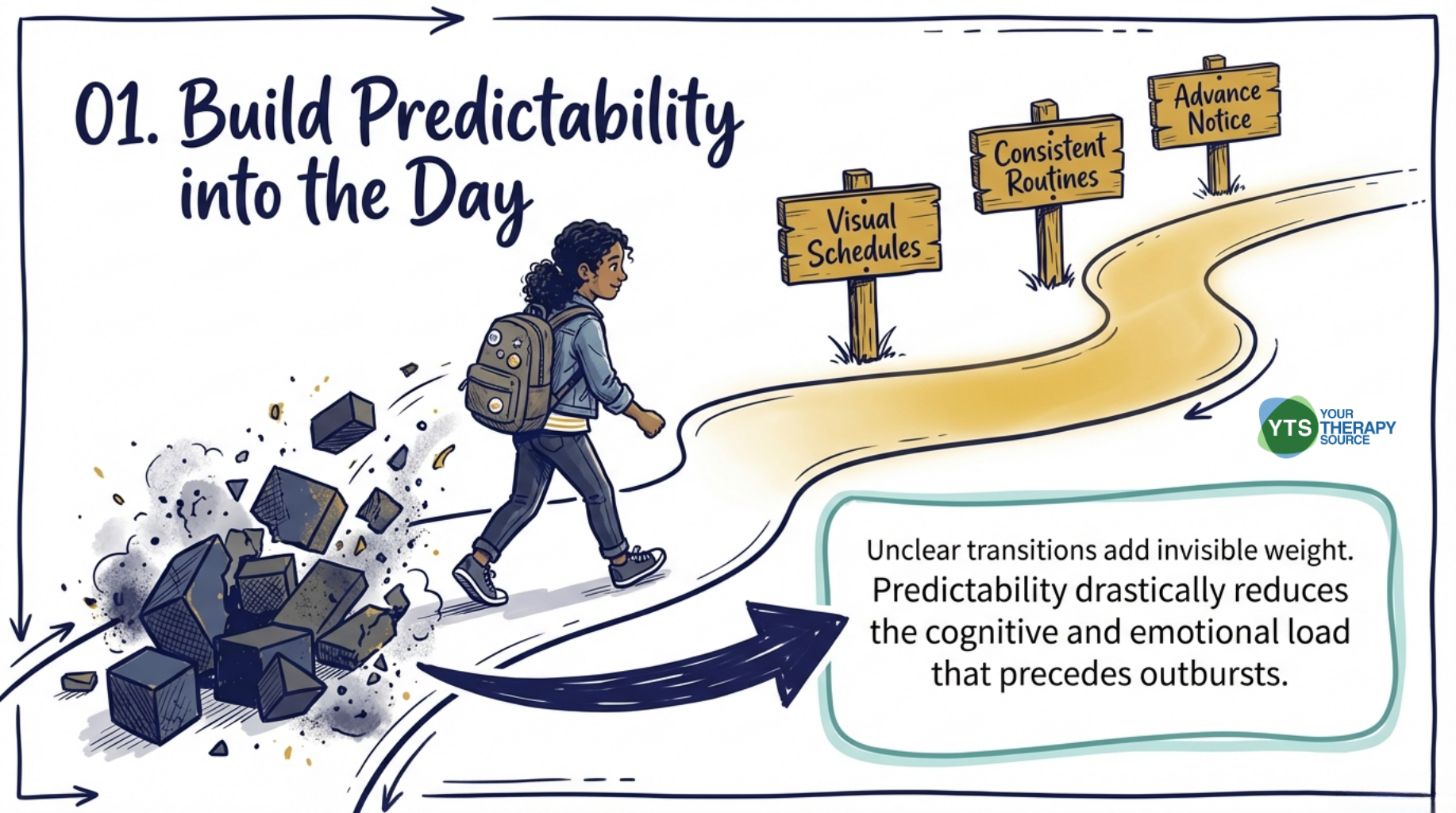
- Build predictability into the school day. Children with ADHD and emotional dysregulation often struggle when transitions or expectations are unclear. Consistent routines, visual schedules, and advance notice of changes can reduce the cognitive and emotional load that tends to precede outbursts.
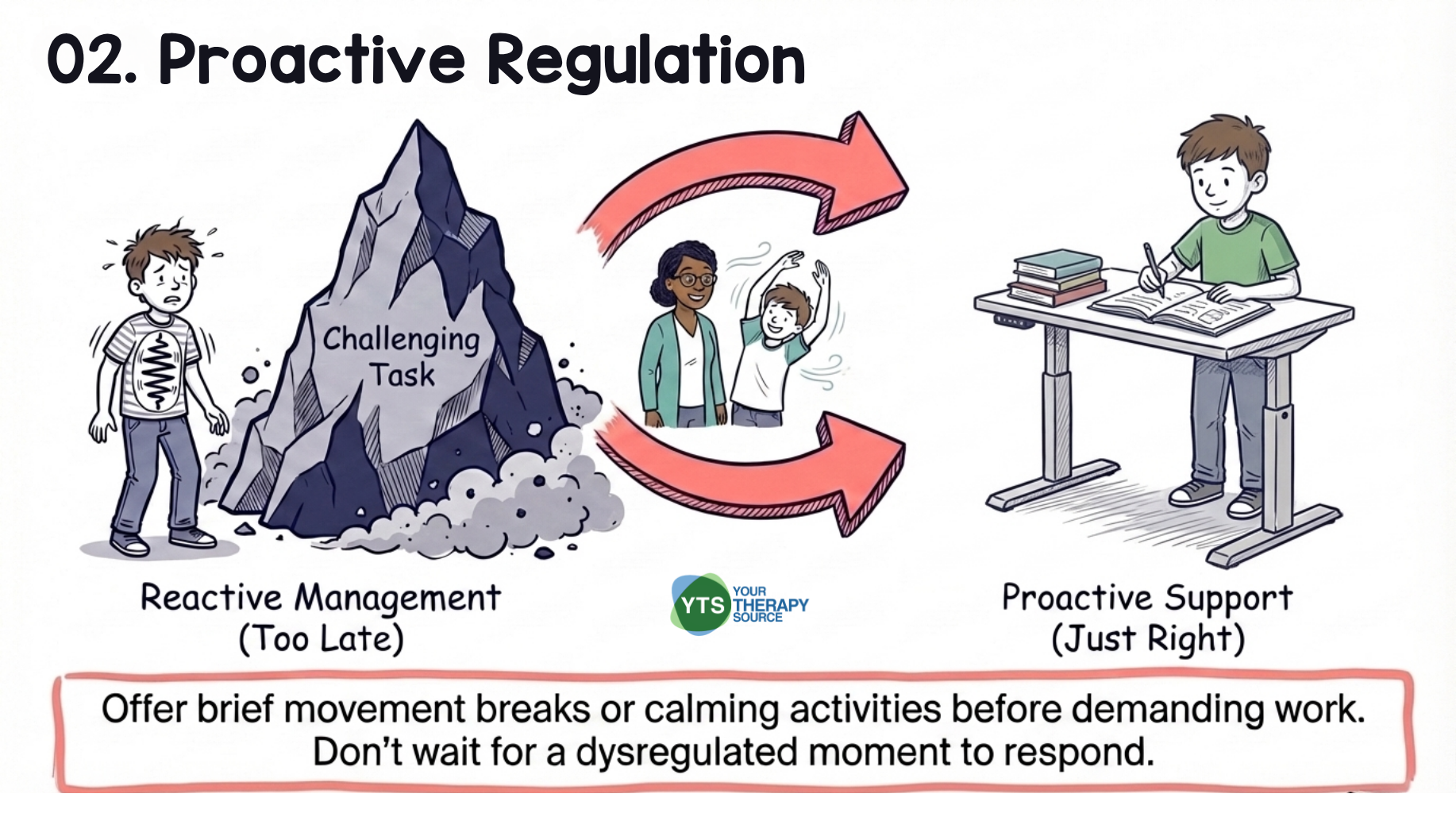
- Create co-regulation opportunities before challenging tasks. Rather than waiting for a dysregulated moment to respond, offer brief movement breaks or calming activities before demanding work. Proactive support is generally more effective than reactive management.
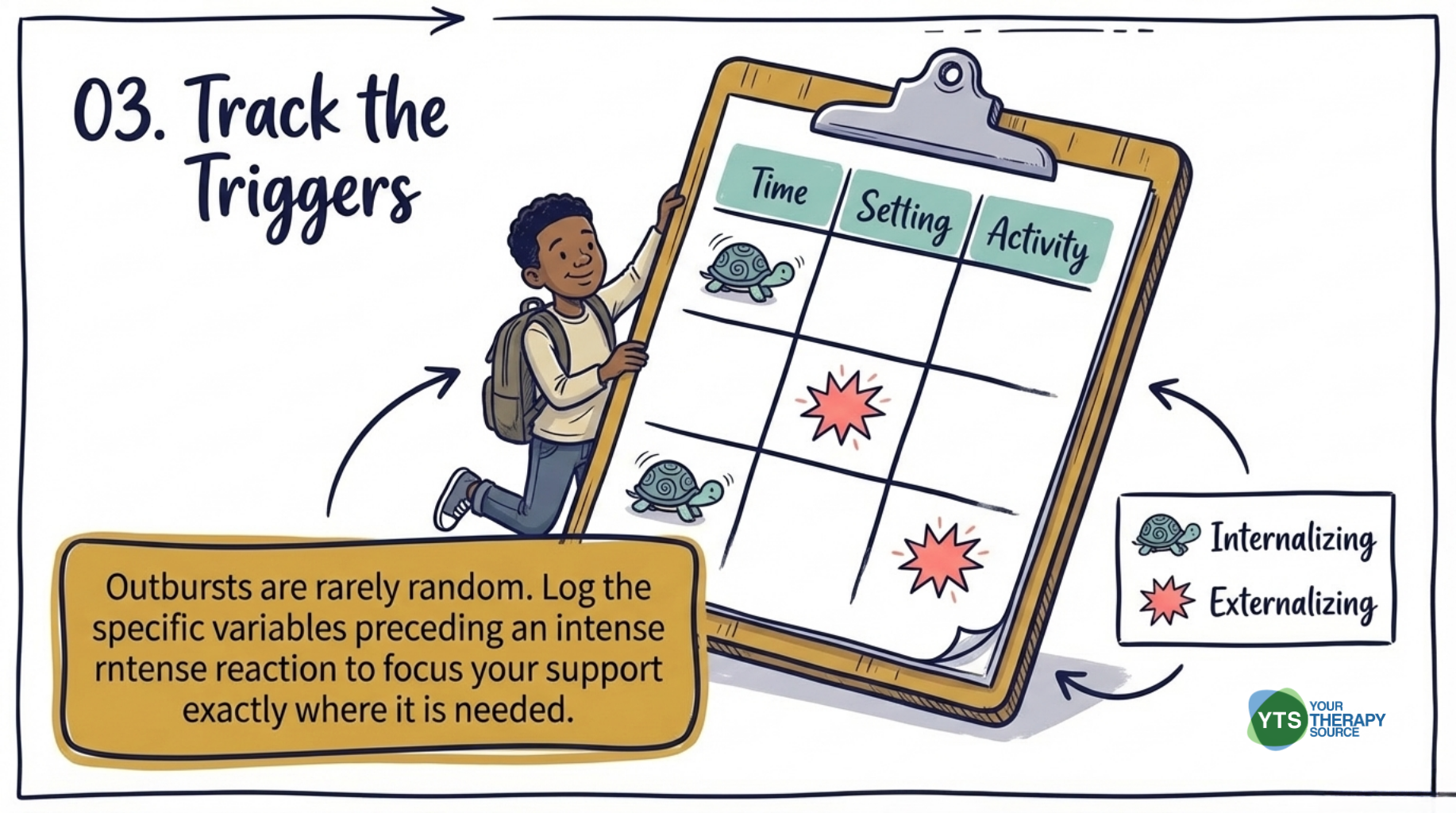
- Observe for patterns in emotional outbursts. Note the time of day, setting, activity type, and triggers that tend to precede intense reactions. Tracking whether a student’s difficulties look more like the externalizing, emotion dysregulation, or internalizing patterns described in this research can help focus support where it is most needed.
- Collaborate with occupational therapists, physical therapists, and school psychologists. The complexity described in this research points to the value of interdisciplinary support. OTs, PTs,psychologists, and educators each bring different tools to understanding and supporting a child’s regulatory needs.
- Incorporate movement into the school day. Physical activity may support executive function and emotional regulation in children with ADHD. Exercise and mental health in children with ADHD is a related area worth exploring when planning school-based supports.
- Use clear and calm language during dysregulated moments. The brain regions identified in this study are involved in processing both attention and emotionally meaningful information. Reducing verbal demands during peak dysregulation can help rather than escalate the situation.
- Support executive function skills explicitly. Children who struggle with emotional regulation often also show difficulty with planning, task initiation, and impulse control. Exercise and ADHD symptoms and executive functions offers additional context on how these skill areas intersect.
- Communicate regularly with families. The study relied heavily on parent report to identify behavioral patterns, which reinforces how much families observe that school staff may not see. Regular, two-way communication supports a more complete picture of the child.
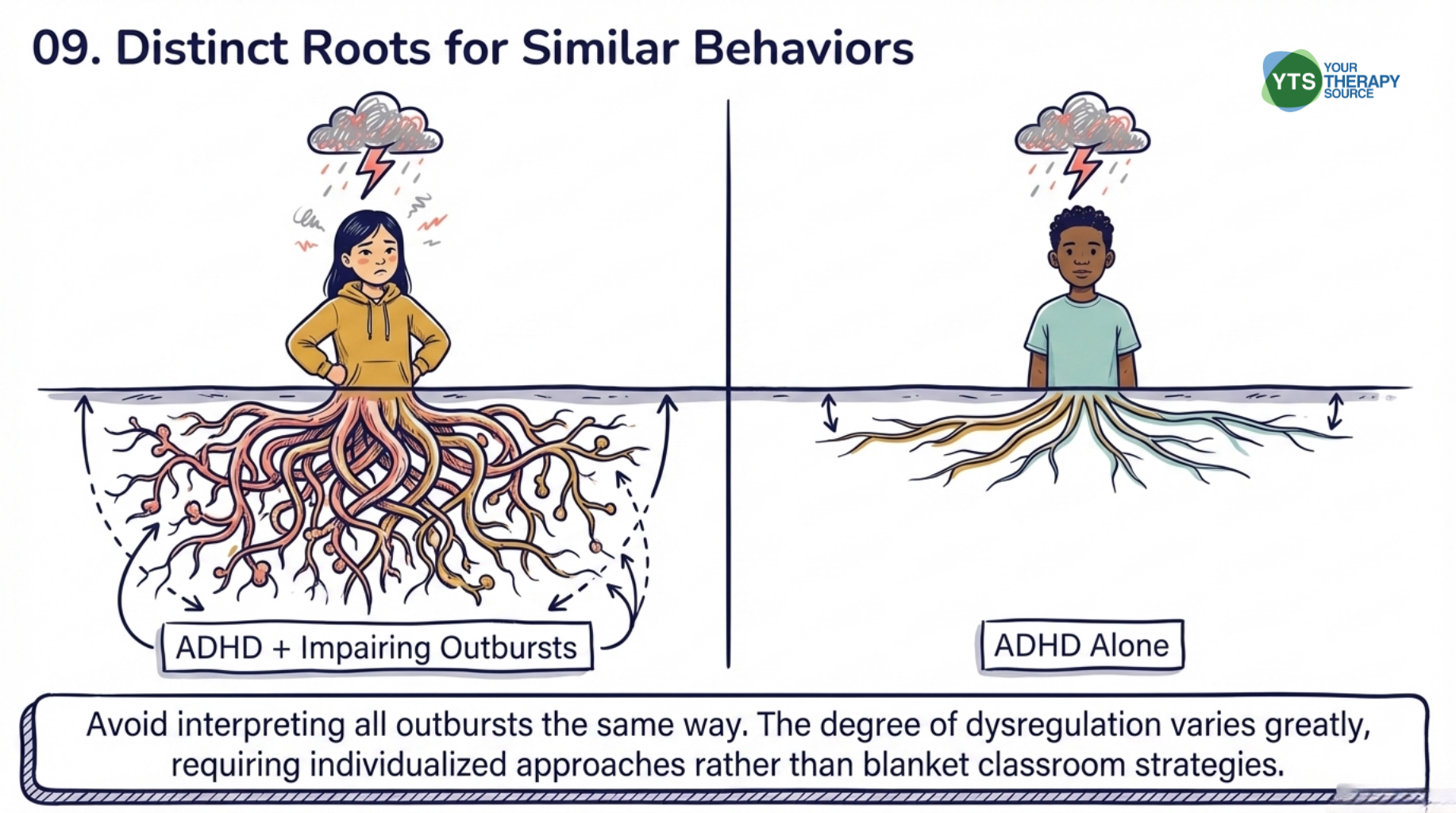
- Avoid interpreting all emotional outbursts the same way. This research found meaningful differences between children with ADHD and impairing outbursts and those with ADHD alone. Not every child with ADHD experiences the same degree of emotional dysregulation, and individualized approaches are more appropriate than blanket strategies.
- Consider organizational support as part of the overall plan. Helping children build structure and predictability in how they manage their day can reduce the cumulative stress that contributes to dysregulation. Tools like an ADHD daily planner can support students in developing routines that reduce cognitive overload.
SUMMARY
This study provides evidence that emotional dysregulation in young children with ADHD may involve distinct patterns of brain structure and connectivity, particularly in regions linked to executive control and attention. Children who experience both ADHD and impairing emotional outbursts show more pronounced externalizing behavior and unique functional brain differences compared to children with ADHD alone. The four behavioral patterns identified in the research offer a useful framework for understanding the range of ways dysregulation can present in school-age children.
For school-based professionals, these findings reinforce the value of looking beyond behavior labels and toward a more complete understanding of each child’s regulatory profile. Thoughtful, individualized, and team-based support that addresses emotional, sensory, and executive function needs together offers the most informed path forward for students who experience these challenges. If you are looking for ready-to-use resources to support self-regulation, movement, and executive function in the classroom, the YTS Action Toolkit offers a practical collection of tools designed for school-based professionals.
REFERENCE
Park, S., Benda, M., Mekhanik, A., Milham, M. P., Hong, S. J., & Roy, A. K. (2026). Mapping latent neuroanatomical substrates of behavioral and emotional dysregulation in ADHD. Psychological Medicine, 56, e48, 1–9. https://doi.org/10.1017/S003329172510278X


